An Inside Look At VP Shunt Surgery. The Courage Within!
It’s been 3 weeks since I had a VP Shunt placed.
There are spots on my skull where it feels like my head has been placed in a vice grip, (stealth machine, to be exact, according to one of the nurses when I asked why I have a covering above my left eye). This video is probably the closest I can get to giving you an idea of what that is. I’ll confirm this at my post op follow-up visit in a few weeks’ time – if I remember.
IMPORTANT: Only watch this next video, if you have the stomach for it.
I also found this VP Shunt placement Go Pro video, which is quite amazing to see, and even more so to realise this is what we endure, and live to tell the tale! I personally had mixed emotions watching it.
*Disclaimer: I am in no way affiliated with the videos shared in this blog. I’m purely sharing for educational and awareness purposes.
Surgery Day: Familiarity comes in many forms
Thinking back to the morning of my surgery; I woke up around 5am with surgery scheduled for 8:30am. I felt extremely dizzy and nauseous, regardless of being upright or lying down. (This had been the case for more than 2 weeks since I had gone to the Emergency Department at the hospital. Thankfully though, on the day of my surgery, the headache that caused my concern and led me there, had subsided and was much more bearable than the throbbing from just a week before). I remember telling myself in the bathroom, “This will all be over in a couple of hours’ time, no more dizziness, no more nausea. Just hang in there.” I gave myself a reassuring smile in the mirror and a hug (because I needed one).
It felt soothing and calming to let the water run over my body. I scrubbed myself from head to toe with the surgical sponge, focusing on the area where my shunt would be placed. (As per Dr Tollesson’s instructions). I had done this (twice) a few days before, as surgery had been planned for earlier in the week but ended up being moved.
To say the week took its toll on me, by the time surgery day arrived, would be an understatement. Preparing yourself mentally, emotionally and spiritually for brain surgery, three times in the space of a few days, just felt torturous. I was truly thankful when Saturday, 23 April arrived.
As thankful as one can be, to have brain surgery, when you have Hydrocephalus.
I packed all my belongings into the hospital bag after showering, and changed into the hospital undies and gown I had been given, preparing to leave the room I had become accustomed to. It was day 11 since entering the hospital.
The corridors to the operating theatres were so familiar to me, having had brain surgery #6, less than 12 months before. It was quite cold, and I was thankful for the insulated blanket the nurse put on my bed as part of the preparation for surgery. “It’s meant to keep you nice and toasty before surgery and helps with finding your veins”, she explained when I asked her about it.
You find solace in the little things
Once the porter parked my bed in the recovery area, a light-hearted interaction with one of the nurses, was comforting and made me smile. He introduced himself as Matthew and told me he would be right there once surgery was over, and looked forward to waking me up. He also said he was going to check to make sure I remembered his name after it was all done. His manner was empathetic, kind and caring – it put me at ease.
I knew what to expect, mostly, which was strangely comforting. I watched as other patients were wheeled in and prepped like me, by the nurses going through their checklists, all waiting for surgery.
There are so many thoughts running through your mind at that time but, somehow, you manage to answer all the same questions the nurses must ask as per hospital protocol, (name, date of birth, any allergies and what are you having done). You’re asked the same questions, by different medical staff, at different times, right up until you’re lying on the operating table. I found myself just going through the motions, and responding, on autopilot.
The anaesthetist (Dr Wong) came into the recovery area and introduced himself. He was personable, jovial even, and managed to make me feel comfortable in his presence. He explained what his role would be (to put me to sleep and ensure I wake up again) and what I could expect to have happen. I gave him the bad news that I have terrible veins, pointing at my arm, and explained that as being the reason why I had a PICC line put in, on the Tuesday (when I thought my surgery was going to happen). Also, when I came into the ED on day one, various nursing staff had 8 attempts at finding a vein, for blood to be taken. The look on his face told me, he knew his work would be cut out for him and said, “That’s ok. We’ll try once you’re under. Shouldn’t feel it then.”. (Apparently, they can’t use a PICC line for anaesthesia, which sucked!). He told me since Dr Tollesson will be “going in through the back” of my head to place the shunt, I will be “placed in a position almost like you’re going for a massage. Come to think of it, that’s exactly what you’ll look like” he said smiling. “If only…” I replied, smiling back at him.
My brain momentarily formulated a picture as I gently pulled my mind away from the thought. A few minutes later my bed was moved to the anaesthesia bay where Dr Tollesson appeared, greeting me with a smile. It was comforting to see a familiar face as my anxiety levels rose. He briefly ran over the plan again at a high-level, I agreed and signed the consent form. I asked him to remember to take a moment of silence, same as last year and he agreed, placing his warm hand over mine, he told me; “Don’t worry, everything will be OK. I’ll take good care of you”. I reminded him (as per his request following our conversation earlier that week) that I didn’t want any staples, and apologised if my request would delay the procedure. I explained that someone had told me it was quicker for the surgeon when they close the incision. He smiled and said, “No, I’m just as quick with my sutures and don’t mind. I haven’t done them in a while but it’s about what you want”.
Once on the operating table, I felt overcome with nausea and dizziness, my guts threatening to spill itself within seconds. I remember thinking what a mess that would make and what it would be like, for the nearly 10 individuals in the room with me. Barely able to get the words out, I asked Dr Wong what he’d given me, and he replied surprised, “Nothing, I haven’t given you anything yet”. Looking at the nurse, he smiled and said, “We haven’t even started yet and already she’s causing trouble”. I took a couple of deep breaths and, in a matter of seconds, I was out…
Post-surgery
Waking up in the recovery room, freezing cold, I started to shake uncontrollably – I was used to this after surgery though. As soon as I was awake enough, I was taken to ICU where I spent the first night. A precaution and standard procedure after having brain surgery with Dr Tollesson. I slept for the next 5 to 6 hours (I think) and one of the first things I recall, when I was awake long enough, is the dizziness, nausea and headache – ALL GONE! I knew it would only be temporary however, I enjoyed it for what it’s worth, how ever long that may last.
I had something to eat, (A sandwich and a cup of tea. Who knew it could taste that good!), despite feeling slightly queasy. Thankfully I was able to sleep more that night. Whatever they gave me during surgery, was strong enough to knock me out for the rest of the evening, in-between observations, of course…
The pain from my incisions only became evident the following day, once I was back in the ward. Running my fingers down my head, over my neck and chest, it felt very tender to touch. Undoubtedly, it was from the tunnelling of the shunt tubing from my head down to my abdomen. I have an incision to the right of my belly button (Just under 8cm long), small scar above my left eye (from the stealth machine), incision down my neck (under my right ear) and a half moon shaped one, on the back of my head. My shunt valve is on the right-side of my head, at the back, slightly higher than my right ear. Working alongside my ETV, which is still wide open.
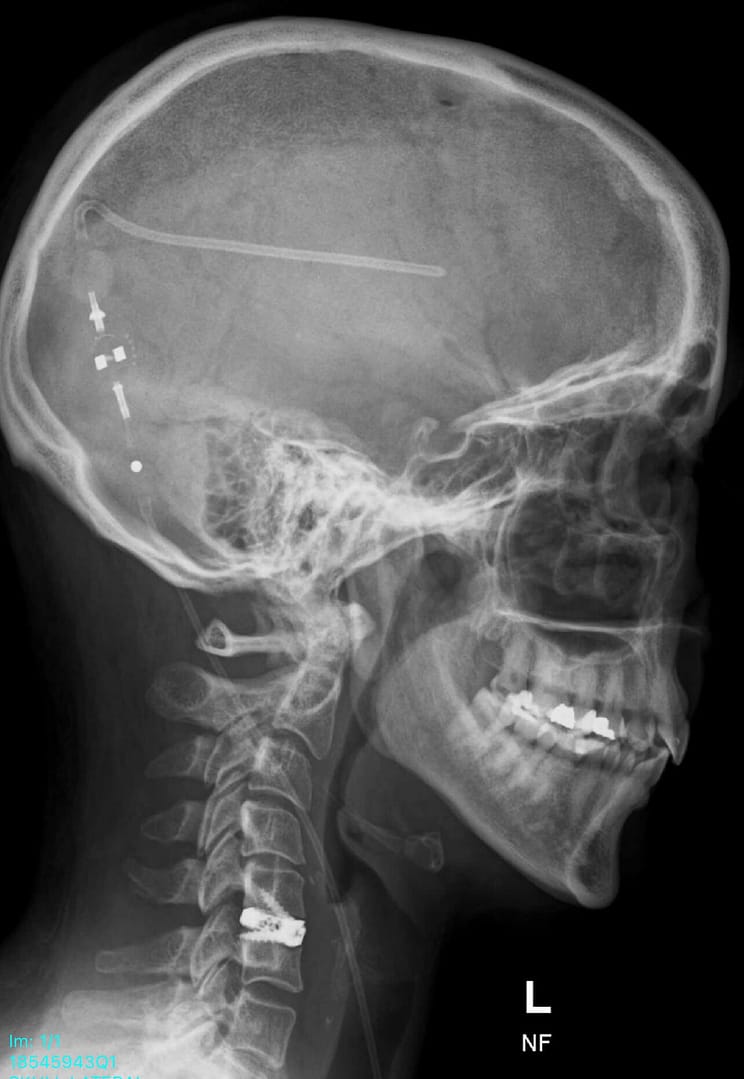


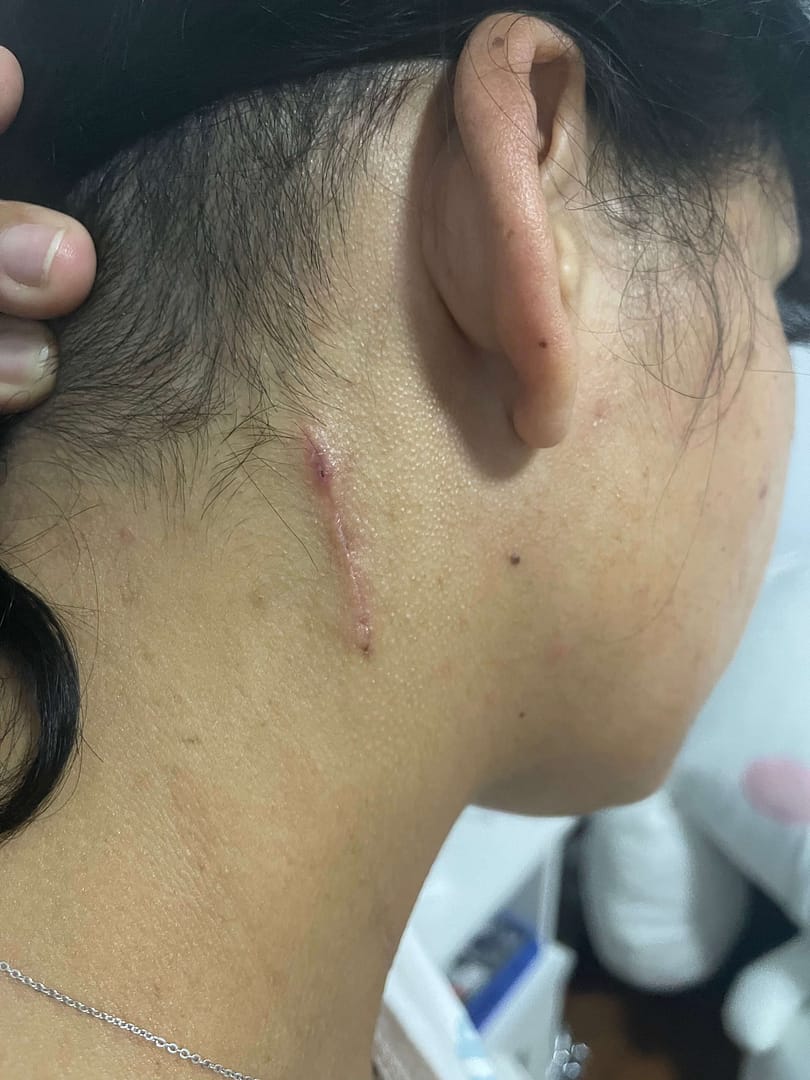
More on my recovery next time…







